
RAISING AWARENESS THROUGH EDUCATION
PROMOTING PREVENTION & EARLY DETECTION CAMPAIGNING FOR CHANGE
SKCIN: THE KAREN CLIFFORD SKIN CANCER CHARITY / REGISTERED CHARITY: 1150048

WE NEED YOUR HELP! PLEASE HELP US TO STOP SKIN CANCER TAKING MORE LIVES. WE ARE HUGELY GRATEFUL FOR YOUR SUPPORT.
Pre-Cancerous Skin Lesions
about each type of skin cancer and what signs of change you should look out for - EARLY DETECTION IS VERY IMPORTANT!
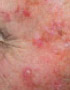
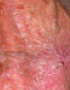
Actinic Keratosis
Actinic Keratosis (AK) is also known as Solar Keratosis caused by UV radiation, is the most common precancer which can advance to Squamous Cell Carcinoma.
- Actinic Keratoses (AK) - also known as Solar Keratoses, (AK, SK) is a common sun-induced, scaly or hypereratotic lesion, which has the potential to beome malignant.
- Actinic Keratosis is the most common precancer - NICE estimates that over 23% of the UK population aged 60 and above have AK.
- Actinic Keratoses are the result of long-term sun exposure and sun damage.
- They are extremely common lesions, especially on the sun-exposed skin of fair-skinned people.
- More than 80% occur on the head and neck, back of the hands and forearms.
- Advancing age, male sex, outdoor occupation or hobbies are all risk factors.
- Although the risk of an AK transforming into squamous cell carcinoma (SCC) is very low, the risk increases over time and with larger number of lesions.
- The presence of ten AK is associated with a 14% risk of developing an SCC within 5 years.
- If you have Actinic Keratoses, it indicates that you have sustained sun damage and could develop any kind of skin cancer - not just Squamous Cell Carcinoma.
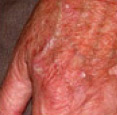
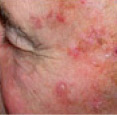
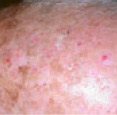
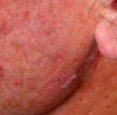
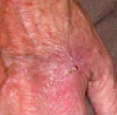
- Usually actinic keratoses appear as scaly or crusty growths that are small, single or multiple rough spots smaller than 1cm in diameter.
- Most become red, but some will be light or dark tan, pink, red, a combination of these, or can be the same colour as your skin.
- They typically present on sun-exposed sites such as the face, scalp, hands and arms
- Actinic Keratoses frequently start so small that they are recognised by touch rather than sight.
- They feel rough (like running your fingers over sand paper) and can cause soreness, irritation, discomfort or pain or they may just pose a cosmetic nuisance.
- You'll most often see the plural, "Keratoses," because there is seldom just one.
- There are many times the number of invisible (subclinical) lesions as visible ones on the skin surface.
- Most often, Actinic Keratoses develop slowly and reach a size from an eighth to a quarter of an inch.
- Early on, these patches may disappear only to reappear later.
- Occasionally they itch or produce a pricking or tender sensation.
- They can also become inflamed and surrounded by redness.
- In rare instances, Actinic Keratoses can even bleed.
- Actinic keratosis is a precancer which indicates sun damage and can lead to Squamous Cell Carcinoma which if left untreated has the potential to spread to organs and be fatal.
Chronic and cumulative sun exposure to the skin is the cause of almost all Actinic Keratosis.
Actinic Kertatosis is frequently seen in patients over 50 due to the cumulative sun exposure over many years, however it is becoming much more common in younger individuals presenting in their 20's and 30's. Tanning and the use of sunbeds increases a persons risk of developing both precancers such as actinic keratosis as well as non melanoma skin cancers and melanoma.
Cumulative UV exposure is the main cause - even on cloudy days (70-80%) of the suns harmful UV rays can pass through cloud) each time an individual spends time in the sun, this adds to the damage which can lead to precancers and skin cancers.
Occasionally, Actinic Keratoses may be caused by extensive exposure to X-rays or a number of industrial chemicals and in individuals whose immune defences are weakened.
Unfortunately, there is no way to know which actinic keratoses are precursors of squamous cell carcinoma. That is why it is important to effectively treat the disorder to eliminate the risk.
The good news is that there are many effective treatments for eliminating Actinic Keratoses.
If Actinic Keratisis is suspected to be an early cancer, it is likely that a sample of tissue will be taken for biopsy. This is done by shaving off the top of the lesion, or scraping it off under local anaesthetic.
Bleeding is usually stopped with a styptic agent. The biopsy is then studied and the best course of treatment will be determined. Sometimes a combination of therapies is advised.
Cryotherapy
Cryotherapy is commonly used when a limited number of lesions exist. Cryotherapy means 'treatment using low temperature', and refers to the removal of skin lesions by freezing them. Many superficial benign lesions can be treated with cryotherapy, but it is most commonly used to remove Actinic Keratoses, Seborrhoeic Keratoses and other small skin cancers such as Basal Cell Carcinomas, Superficial Squamous Cell Carcinoma and Bowen's Disease.
The tumour tissue is destroyed by freezing it with liquid nitrogen, this is done by using a spray device or cotton-tipped applicator. Cryotherapy does not normally require a local anaesthetic and it involves no cutting or bleeding, the procedure itself lasting a matter of seconds.
The area of frozen skin will turn white, thawing to normal skin temperature within a couple of minutes. The procedure may be repeated to ensure the eradication of all malignant cells.
Swelling, redness and blistering can occur following treatment.
The growth then scabs and falls off within weeks.
The treated area will usually look normal once healed, but some scarring can or discoloration can occur particularly on the legs or on darker skinned patients. (It is important not to pick the wound during healing). This treatment has a lower overall cure rate than surgical methods but may be a treatment of choice for some patients.
Surgical Excision
Generally surgery is unnecessary but there are exceptions. Bleeding, induration, rapid growth, or pain suggest progression to SCC or when AK are very thick or resemble cutaneous horns, hyperkeratotic AK, or where invasive squamous cell carcinoma is suspected or diagnosis is in doubt.
A local injection into the affected skin is administered with anaesthetic. The actinic keratosis can then be scraped off with a sharp spoon-like instrument (a curette), or cut out and the wound closed with stitches. Surgical removal does leave a scar but it also provides a specimen that can be analysed in the laboratory to confirm the diagnosis.
Example of Wide Local Excision
of Bases Cell Carcinoma. Patient: John Holmes

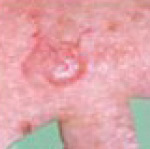
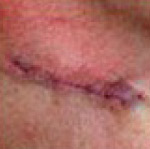
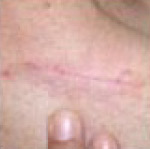
Curettage and cautery
This is a �scrape and burn� technique that uses a curette to mechanically scrape away the AK's atypical cells then cauterises the base and is an excellent way to treat AK. It offers high cure rates with excellent cosmetic outcomes. It is a safe and effective treatment for Actinic Keratosis.
Curettage is effective for almost all clinical types of AK but is particularly useful for those lesions thought to be closer to invasive squamous cell carcinoma (SCC), lesions resistant to other treatments, and after biopsy. Disadvantage of curettage is that a local anaesthetic is required. If the skin is burned too rigorously a scar can result. Infection and other complications are rare.
Topical Medications
Topical medications consist of courses of creams containing drugs which may include 5-fluorouracil, Imiquimod or Ingenol Mebutate gel which are useful treatments for Actinic Keratoses, especially if there are many of them.
These preparations appear to selectively destroy the abnormal cells in sun-damaged skin.
However, they can cause a lot of temporary inflammation of the treated areas.
For milder cases of Actinic Keratosis Diclofenac and retinoic acid are other drugs in cream or ointment form that are helpful.
What are the side effects of creams and gel treatments for AK?
Local skin reactions (also known as "LSRs") occurring where creams and gels are applied are very common. The skin may develop redness, peeling, swelling and scabs for a period of days or weeks during the healing process. The length of time these reactions persist will depend partly on the treatment chosen. Discuss your options and what to expect from your treatment with your doctor. You may want to plan to start the treatment when these reactions - particularly on visible areas - will cause you the least inconvenience.
Chemotherapy - 5-FU, Efudix
This is a safe and highly effective treatment for AK with cure rates up to 93%.
5-FU spares normal skin but can �light-up� clinically unapparent or early AK.
However, treatment can be long (The usual duration of initial treatment 3-4 weeks) and produce inflammation at the site of the AK resulting in prolonged redness and unsightly and sore erosions.
It is also available as Efudix cream and suited to the treatment of multiple AKs.
Unfortunately lower cure rates are reported when patients cannot comply or the medication is used improperly. Treatment failures as high as 60% have been reported.
Sunlight can cause pain and discomfort at the sites being treated.
Photodynamic Therapy (PDT)
Photodynamic therapy or PDT is a relatively new type of treatment and an alternative to surgery in some cases. It is basically treatment with a chemical that makes the skin cells sensitive to light and when the area to be treated is exposed to laser light, the cells die off.
It is best used on thinner skin cancers, in cases where you would need a lot of surgery and can be especially useful for growths on the face and scalp. It is not suitable for deeper skin cancers because the light cannot penetrate far enough into the skin.
PDT is now available on the NHS for Bowen's Disease, basal cell skin cancers and Actinic Keratosis (Solar Keratosis), but is not available in all hospitals.
To have this treatment, you first have the crust and scale removed from your skin lesion, you then have a cream that contains light sensitising chemical applied to the affected and surrounding area. Sometimes, you may have this chemical as a tablet or injection. After the drug has been absorbed, you will have a strong light shone on to the treated area for up to 45 minutes. The light will kill any cell that has absorbed the drug. This treatment is likely to be repeated more than once.
Redness and swelling are common side effects. After treatment, patients become locally photosensitive for 48 hours where the light sensitizing chemical was applied, and must avoid the sun.
Laser treatment
Laser treatment may be useful particularly for actinic keratosis in small or narrow areas, and, therefore, can be particularly effective for Keratoses on the face and scalp, as well as Actinic Cheilitis on the lips. A carbon dioxide or erbium YAG laser is focused onto the lesion, and the beam cuts through tissue without causing bleeding. Local anaesthetic may be necessary, and some pigment loss can occur. Laser treatment is a useful options for people taking blood thinners or as a secondary treatment when others have not succeeded.
Field change refers to areas of skin that have multiple AK associated with a background of erythema, telangiectasia and other changes seen in sun-damaged skin. Patients with this are likely to be more at risk of developing SCC (risk is greater if left untreated) it is therefore recommended that patients should be treated more vigorously with treatment applied to the whole area of field change, not just individual lesions.
The primary aim of treatment is to reduce the total number of lesions that the patient has at any one time to reduce the risk of developing SCC. Treatment courses will need to be repeated from time to time. All field based treatments will elicit local skin responses, which are expected as part of the treatment - these responses will vary widely between the treatments outlined below.
For smaller areas of field change (for example an area the size of a palm or most of the forehead) the following treatments should be considered:
Aldara ® cream (5% Imiquimod)
Used three nights a week (for example Monday, Wednesday and Friday) for four weeks.
It is applied overnight and washed off the following morning.
After the treatment the use of a mild topical steroid eg 1% Hydrocortisone or Eumovate ® cream BD will be considered for a two to four week period to help settle down any inflammation.
A follow up three months after the treatment was started, will indicate if the treatment needs to be repeated.
Advantages - generally very effective in terms of clearance, and cosmetic appearance once inflamation is resolved.
Disadvantages - patients should be warned to expect marked erythema with crusting of the skin. Timing of the treatment is an important consideration as some patients develop flu-like symptoms during treatment.
Efudix ® cream (5-FU)
Used once a day for four weeks.
Applied thinly in an evening with a gloved finger.
The treated area should be washed the following morning.
After the treatment the use of a mild topical steroid eg 1% Hydrocortisone or Eumovate ® cream BD will be considered for a two to four week period to help settle down any inflammation.
Follow up three months after the treatment was started
Advantages and disadvantages similar to with Aldara ®, although patients do not develop flu-like symptoms.
Picato® (ingenol mebutate) Gel
This is a new treatment with similar outcomes to the above, however in addition it benefits the patient with a very short treatment period in comparison to the other topical treatments.
For the face and scalp - the formula is applied for 3 consecutive days only.
For the trunk and extremities - for 2 consecutive days only
This treatment is suitable for thin patches (also known as "lesions") of actinic keratosis. It is usually used to treat a single area of Actinic Keratosis (equivalent to 5x5cm) containing multiple patches of actinic keratosis. The gel is supplied in small individual tubes. Each tube contains enough gel for a single daily application. The gel is applied for 3 days on the face/scalp, or 2 days on other body areas. LSRs typically resolve within 2 weeks on the face/scalp and within 4 weeks on other body areas. This treatment can be prescribed by either a GP or a dermatologist.
For further information on Picato® please download the Patient Information Leaflet (PIL) below. This is the leaflet included in the pack with a medicine. It is written for patients and gives information about taking or using a medicine. However, it is possible that the leaflet in your medicine pack may differ from this version because it may have been updated since your medicine was packaged.
Download Picato® Patient Information Leaflet >
Photodynamic therapy
This is provided by some dermatology departments and occasionally GPwSI clinics.
A single treatment is often provides effective for an area of field change. The skin settles down within a few days of treatment and cosmetic outcomes are good.
For larger areas of field change the following treatments should be considered:
Solaraze ® gel (3% Diclofenac in Sodium Hyaluronate)
Used twice a day for 12 weeks with patient review after four weeks to assess response.
Advantages - generally well-tolerated and can therefore be used on any sized area.
Disadvantages - most dermatologists view Solaraze as a milder treatment, so is best used where the AK are thin.
Prevention is better than cure.
Whilst most skin cancers and precancers are curable if detected early, prevention is always better than cure. 80-90% of all skin cancers can be avoided by ensuring that appropriate precautions are
taken during time spent in the sun.
Always follow the five S's of sun safety below and make sure you stick to these golden rules:
- Avoid tanning and never allow your skin to burn
- Never use indoor tanning devices
- Examin your skin thoroughly at least once a month
- If you are worried or uncertain about any abnormality, seek immediate professional advice
For those that have suffered from a precancer, or skin cancer, particular care and attention to covering up and shading from the sun is very important as well as thoroughly checking your skin more frequently for signs of recurrence or developments of new abnormalities.
The Five S's of Sun Safety:

SLIP on a T-shirt
Always keep shoulders covered
as they can easily burn in the sun

SLOP on good quality sunscreen
Always use a sunscreen with a minimum SPF of 30 with broad spectrum UVA protection
Apply generously 20 mins before going outside and reapply at least every 2 hours

SLAP on a broad brimmed hat
Wear a legionnaire or broad-brimmed hat to help shade the face, neck and ears
which can easily burn in the sun.

SLIDE on quality sunglasses
Wear quality (preferrably wrap-around) sunglasses to help protect
your eyes that can be damaged by the sun.

SHADE - Seek shade whenever possible
Always seek shade, particularly between 11am and 3pm when the sun's
UV penetration is strongest.
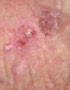

Intra-Epidermal Carcinoma (Bowen's Disease)
Bowen's Disease is a precancerous skin lesion that has not yet penetrated the basement membrane, but can if left untreated, lead to Squamous Cell Carcinoma.
- Bowen's disease = Intraepidermal Carcinoma = IEC = Squamous cell carcinoma in-situ.
- Bowen's disease is a precancerous lesion. In-situ refers to the fact that the disease has not penetrated the basement membrane. Once this occurs, the lesion is a Squamous Cell Carcinoma - a full blown skin cancer.
- Bowen's disease typically presents as an asymptomatic, slow growing, sharply-demarcated, scaly erythematous [red, pink, salmon coloured] patch or plaque. The border may be irregular.
- The surface may be flat, scaly, crusted, eroded, ulcerated, velvety or verrucous [warty].
- Because of its asymptomatic nature, lesions may become very large by the time of presentation.
- Although Bowen's disease can occur just about anywhere, common sites for presentation are the lower limbs and head and neck.
- Bowen's disease occurs most commonly in later life and most patients aged over 60.
- Women are affected more than men.
- In approx. 3% of cases Bowen's disease transforms to squamous cell carcinoma and about 1/3 of these will metastasise [spread to other parts of the body] and become fatal.
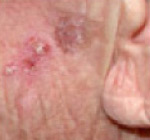
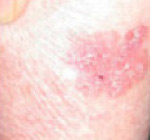
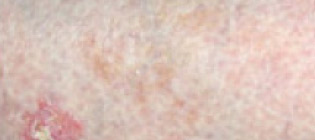
- A patch of Bowen's disease starts as a small red scaly area, which grows very slowly.
- Often there are no symptoms, although the surface may catch on clothing.
- It may reach a diameter of a few centimetres across.
- It commonly occurs on sun-exposed skin, especially the face, scalp and neck, as well as the hands and lower legs, but can occur anywhere. More than one area may be present.
- Bowen's disease typically presents as an asymptomatic, slow growing, sharply-demarcated, scaly red, pink, salmon coloured patch or plaque. The border may be irregular.
- The surface may be flat, scaly, crusted, eroded, ulcerated, velvety or verrucous [warty].
The development of an ulcer or lump on a patch of Bowen's disease may indicate the formation of invasive squamous cell cancer, so it is very important to seek professional advice with anything suspicious.
- The majority of cases of Bowen's Disease develop as a result of long-term sun exposure which is why it commonly presents on areas regularly exposed to the sun.
- Due to long term sun exposure, it typically presents in older individuals with a higher cumulative exposure to UV radiation, but can present in younger adults.
- Bowen's Disease is not hereditary, but some of the factors that increase the risk of getting it, such as a fair skin and a tendency to burn in the sun, do run in families.
- Bowen's Disease is not infectious, nor due to an allergy.
- Bowen's Disease is more likely in those receiving long term immunosuppression medication.
- Very occasionally, Bowen's Disease may be seen following: radiotherapy, longstanding arsenic ingestion (very rare nowadays) or on the genitals in association with the virus that causes
warts (the human papillomavirus).
A particular problem with Bowen's Disease is that it is frequently found on the lower leg.
The skin there is often tight and sometimes quite fragile, especially in older patients.
Healing there is slow. Many factors, therefore, play a part in selecting the right treatment including:
- The size and thickness of the patch
- The number of patches
- The presence of swelling of the legs
- The general condition of the skin on the legs
- The patient's preference
No treatment?
Given that only 3% of Bowen's Disease progresses to invasive squamous cell carcinoma then no treatment could be considered an option. Lesions especially suitable for no treatment are those that are thin and considered unlikely to progress to squamous cell carcinoma and those located on sites where healing is a problem. If the affected area is judged to be thin and not likely to cause problems, your dermatologist may simply suggest that it is kept under observation in a clinic, or in some cases by yourself or by your GP. This can be common in some elderly, frail patients with co-morbidity or with a limited lifespan. In other words, it may be kinder to do nothing.
Topical Medications
Fluorouracil [5FU 5%cream = Efudix] Several open studies have shown 5FU to be efficacious in clearing Bowen's Disease. Cure rates of 66-93% have been reported.
The highest cure rates are achieved when Efudix is applied once or twice daily for 6-16 weeks and included a margin around the lesion.
There is a lot of variability in the way Efudix is prescribed with some Physicians recommending it twice a day, every day, others every other night or twice weekly and for differing lengths of treatment.
Efudix sometimes produces irritation, inflammation, erosions and ulcerations, so less aggressive regimens have been suggested. But these regimens give higher recurrence rates.
Imiquimod (Aldara) Cream. This was originally developed for the treatment of genital warts, but Imiquimod cream has been found useful in treating Bowen's Disease.
This is an immune response modifier, rather than inhibiting and suppressing the immune system it stimulates it - demonstrating potent antiviral, anti-tumour and immunoregulatory properties.
In one study, 16 patients with Bowen's disease applied Imiquimod over 16 weeks.
Lesions were up to 5.5 cm in diameter. 15 legs 1 shoulder 6 weeks after treatment 14/15 patient's biopsies showed no residual tumour. Patients did experience local skin reactions similar to
5-fluorouracil and 6 patients stopped early because of local skin reactions.
Cryotherapy
Cryotherapy is commonly used when a limited number of lesions exist. Cryotherapy means 'treatment using low temperature', and refers to the removal of skin lesions by freezing them. Many superficial benign lesions can be treated with cryotherapy, but it is most commonly used to remove Actinic Keratoses, Seborrhoeic Keratoses and other small skin cancers such as Basal Cell Carcinomas, Superfi�cial Squamous Cell Carcinoma and Bowen's Disease.
The tumour tissue is destroyed by freezing it with liquid nitrogen, this is done by using a spray device or cotton-tipped applicator. Cryotherapy does not normally require a local anaesthetic and it involves no cutting or bleeding, the procedure itself lasting a matter of seconds.
The area of frozen skin will turn white, thawing to normal skin temperature within a couple of minutes. The procedure may be repeated to ensure the eradication of all malignant cells.
Swelling, redness and blistering can occur following treatment.
The growth then scabs and falls off within weeks.
The treated area will usually look normal once healed, but some scarring can or discoloration can occur particularly on the legs or on darker skinned patients. (It is important not to pick the wound during healing). This treatment has a lower overall cure rate than surgical methods but may be a treatment of choice for some patients.
The benefits of cryotherapy should be balanced against the risk of creating an ulcer that may take a long time to heal (e.g. BD on lower leg of elderly female).
Surgical Excision
For well-defined small lesions where excision and primary closure can be performed surgery is a good option. But one has to be careful as lesions on the lower leg can be large and the skin is poorly vascularised skin where healing can be a problem one risks dehiscence or necrosis or skin grafting adding to morbidity. The recurrence rates for Bowen's disease removed by simple excision is between = 5 -20% and may be related to subclinical extensions.
Generally surgery is unnecessary but there are exceptions. Bleeding, induration, rapid growth, or pain suggest progression to SCC and may be recommended where invasive squamous cell carcinoma is suspected or diagnosis is in doubt.
A local injection into the affected skin is administered with anaesthetic. The affected area can then be scraped off with a sharp spoon-like instrument (a curette), or cut out and the wound closed with stitches. Surgical removal does leave a scar but it also provides a specimen that can be analysed in the laboratory to confirm the diagnosis.
Mohs micrographic surgery
Mohs micrographic surgery is most commonly used to remove basal cell carcinomas, but can sometimes be used to remove other tumours or larger lesions, or where tissue sparing is vital eg younger patients but expensive and time consuming. Recurrence rates are lower with Mohs micrographic surgery. Generally not needed for Bowen's Disease except at critical sites or after recurrences.
During Mohs surgery, using a scalpel the visible tumour is removed along with a very thin layer of tissue surrounding it. This layer is then checked immediately and thoroughly under a microscope.
If the atypical cell are still present in or around the surrounding tissue, the procedure is repeated until eradication. The wound is then stiched and after surgery, the wound may be allowed to heal naturally or if necessary be reconstructed using plastic surgery methods.
Example of Mohs Micrographic Surgery:
Removal of Basal Cell Carcinoma. Patient: Richard Clifford
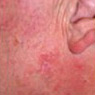
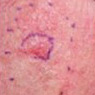
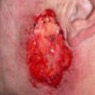
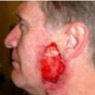
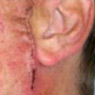
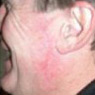
Curettage and cautery
This is an excellent treatment for Bowen's disease. Its a simple, quick and inexpensive procedure and high cure rates have been quoted.
Generally cure rates are similar to other treatments with some advantages. A report in the British Journal of Dermatology a few years ago showed the superiority of curettage and cautery over cryotherapy in the treatment of Bowen's Disease especially lower leg.
In selected cases curettage and cautery can give shorter healing times with less pain, fewer complications and lower recurrence rates than cryotherapy.
Recurrences may be attributable to the experience of the surgeon or to repopulation by Bowen's Disease cells from hair follicles, sweat gland etc.
Curettage and cautery is a "scrape and burn" technique that uses a curette to mechanically scrape away the atypical cells then cauterises the base. It offers high cure rates with excellent cosmetic outcomes. It is a safe and effective treatment for Bowen's Disease.
Curettage is particularly useful for those lesions thought to be closer to invasive squamous cell carcinoma (SCC), lesions resistant to other treatments, and after biopsy.
Disadvantage of curettage is that a local anaesthetic is required. If the skin is burned too rigorously a scar can result. Infection and other complications are rare.
Radiotherapy
Bowen's disease is reported to be radiosensitive, various forms of ionising radiation have been used and cure rates = 89-100%
Advantages are: Management of large and multiple lesions - especially in elderly, infirm or those on anticoagulants [blood thinners]
Disadvantages are: Radionecrosis, Inadequate treatment at deep margin leads to recurrences
Problem with healing - especially lower leg. Poor healing associated with diameter of radiotherapy field, dosage and energy of radiation, patient age >90
Photodynamic therapy [PDT]
In the last decade PDT has shown considerable promise for the treatment of premalignant skin conditions such as Bowen's disease.
A topical photosensitiser precusor is applied to a lesion this is preferentially taken up by tumour cells and converted to a potent photosensitiser the lesion is then irradiated with light activating the photosensitiser and the tumour is destroyed.
Several studies have shown topical PDT to be effective in the initial clearance of Bowen's Disease.
Cosmetic results are usually excellent consider it for: large lesions, on poorly vascularized skin or for those patients unsuitable for surgery. But it is time consuming and repeated treatments can be
necessary.
Laser treatment
Laser treatment may be useful particularly for Bowen's Disease in small or narrow areas, and, therefore, can be particularly effective for areas affecting the face and scalp. A carbon dioxide or erbium YAG laser is focused onto the lesion, and the beam cuts through tissue without causing bleeding. Local anaesthetic may be necessary, and some pigment loss can occur. Laser treatment is a useful options for people taking blood thinners or as a secondary treatment when others have not succeeded.
Prevention is better than cure.
Whilst most skin cancers and precancers are curable if detected early, prevention is always better than cure. 80-90% of all skin cancers can be avoided by ensuring that appropriate precautions are
taken during time spent in the sun.
Always follow the five S's of sun safety below and make sure you stick to these golden rules:
- Avoid tanning and never allow your skin to burn
- Never use indoor tanning devices
- Examin your skin thoroughly at least once a month
- If you are worried or uncertain about any abnormality, seek immediate professional advice
For those that have suffered from a precancer, or skin cancer, particular care and attention to covering up and shading from the sun is very important as well as thoroughly checking your skin more frequently for signs of recurrence or developments of new abnormalities.
The Five S's of Sun Safety:

SLIP on a T-shirt
Always keep shoulders covered
as they can easily burn in the sun

SLOP on good quality sunscreen
Always use a sunscreen with a minimum SPF of 30 with broad spectrum UVA protection
Apply generously 20 mins before going outside and reapply at least every 2 hours

SLAP on a broad brimmed hat
Wear a legionnaire or broad-brimmed hat to help shade the face, neck and ears
which can easily burn in the sun.

SLIDE on quality sunglasses
Wear quality (preferrably wrap-around) sunglasses to help protect
your eyes that can be damaged by the sun.

SHADE - Seek shade whenever possible
Always seek shade, particularly between 11am and 3pm when the sun's
UV penetration is strongest.
THE EARLY DETECTION OF SKIN CANCER CAN REDUCE YOUR RISK OF POTENTIAL DISFIGURMENT OR EVEN DEATH.
Make sure you check your skin thoroughly at least once a month for signs of change.
Remember what to look out for when checking your skin - download and print off our early detection fact sheet.
DOWNLOAD NOWREMEMBER: If you are worried or uncertain about any suspicious patch, lump, mole or lesion - go to your GP and seek professional advice from a skin specialist or dematologist immediately.
REMEMBER: PREVENTION IS BETTER THAN CURE!
Always use the
Five S's of Sun
Safety & never allow
your skin to burn!







